The structure of our residency program supports the unique learning needs of each individual resident.
Individualized curriculum
Evaluation and feedback
Effective feedback includes both formative and summative components that are tailored to the learner's specific learning needs and perspective. Opportunities for frequent on-the-fly coaching and progressive feedback are created by the close relationships between our faculty and residents.
Rotation directors meet with residents regularly throughout each rotation to discuss summative feedback and ongoing learning goals. Evaluations are based on multiple sources of input from various members of the healthcare team, including:
- Direct observation of patient care
- Oral presentations on rounds
- Review of documentation; staff and nursing comments
- Patient satisfaction surveys
Simulation opportunities
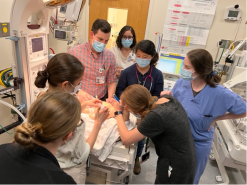
Simulation training is at the forefront of medical education. Our pediatric residency incorporates regularly scheduled simulation sessions into the curriculum. These sessions provide experiential opportunities that mirror real-life situations in an interactive method. The experience incorporates direct feedback and reflective learning, both hallmarks of adult learning.
We utilize our state-of-the-art simulation center for many activities, including resident mock code training for both pediatric and neonatal scenarios, third- and fourth-year medical student sessions, resident small group procedural sessions, and participation in multiple simulation research and quality improvement projects. We also have a simulation curriculum that each resident is expected to complete on a yearly basis to ensure adequate training in pediatric procedures and resuscitation.
Simulation benefits
- Provides a safe environment where mistakes do not cause patient harm.
- Exposure to rare but complicated events.
- Ability to tailor the level of difficulty to individual learners' needs.
- Stimulating immediate feedback.
- Encouraging repetitive and deliberate practice.
- Fostering team training.
Preventive Medicine Residency Program
The Pediatrics Preventive Medicine Residency Program is a special two-year program offered in conjunction with the Dartmouth Institute for Health Policy and Clinical Practice at Geisel School of Medicine at Dartmouth. A successful completion results in a Master's of Public Health degree from Dartmouth as well as board eligibility in Pediatrics and in Preventive Medicine.
The program is structured as a leadership track option for those Dartmouth residents taking a clinical residency who wish to gain further knowledge and skills in the measurements of outcomes and the leadership of change and improvement in health care systems. Residents are accepted into the master's track by competitive application after joining the pediatric residency program.
About the Dartmouth Institute for Health Policy and Clinical Practice (TDI)
TDI is a dynamic force within Dartmouth College, dedicated to improving health care through education, research, policy reform, leadership improvement, and communication with patients and the public.
Learn more about TDI initiatives and research on the TDI website